 The Centers for Medicare and Medicaid Services today announced release of the 2015 Impact Assessment of Quality Measures Report. Designed to relate the performance on quality measures over time, it includes research on 25 quality programs and hundreds of quality measures from 2006 to 2013.
The Centers for Medicare and Medicaid Services today announced release of the 2015 Impact Assessment of Quality Measures Report. Designed to relate the performance on quality measures over time, it includes research on 25 quality programs and hundreds of quality measures from 2006 to 2013.
Key findings of the report include:
Overall quality measurement results demonstrate significant improvement over time.
Race and ethnicity disparities present in 2006 were less evident in 2012.
Provider performance on CMS measures related to heart and surgical care saved lives and averted infections.
CMS quality measures impact patients beyond the Medicare population.
CMS quality measures support the aims of the National Quality Strategy (NQS) and CMS Quality Strategy.
There is an old management adage that goes, “what cannot be measured cannot be managed.” It is from this vantage that CMS advocates for the role quality measurement plays in achieving the desired goals of improved access, better outcomes and lower cost (the infamous Triple Aim liberally interpreted by me). While the data may support improvement in performance indicators, that does not necessarily translate into value.
And value is (or ought to be) the universal currency of the Triple Aim
Recall, I have shared here often that value in healthcare is defined as outcomes divided by cost – and that measuring outcomes is a bit like trying to nail Jell-O to the wall. Measuring and reporting on quality in other industries has proven to be a useful endeavor that underpins market efficiencies. It’s not the availability and use of information derived from such endeavors that I wonder about – but who uses it and how.
Consumers that are armed with information on product and service quality from organizations like Consumer Reports are better able to navigate the value paradigm and reconcile their wants and needs against affordability. But in healthcare, consumers (patients) largely still don’t get to do that regardless of how much Big Data is collected, analyzed and reported on by CMS.
Will future efforts to capture all of the nuances that influence how individuals determine the value of an outcome ever be adequately captured by Big Data analytics in a fashion that such knowledge can supplant the simple effectiveness of personal decision making in a free market? CMS is banking on it.
What say you?
Cheers,
~ Sparky





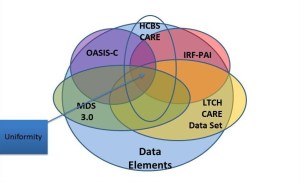




 For those policy wonks out there looking for resources to support your work here is a phenomenal publication that you need to be familiar with.
For those policy wonks out there looking for resources to support your work here is a phenomenal publication that you need to be familiar with.  Back in the day, before Al Gore had even understood the full impact of his new invention, the Internet was raw and without form. It took the efforts of early technology pioneers who could envision the scalability and acceleration of historic processes. Eric Thomas was an engineering student in Paris back in 1986 when he invented a software program that automated the management of email lists: LISTSERV.
Back in the day, before Al Gore had even understood the full impact of his new invention, the Internet was raw and without form. It took the efforts of early technology pioneers who could envision the scalability and acceleration of historic processes. Eric Thomas was an engineering student in Paris back in 1986 when he invented a software program that automated the management of email lists: LISTSERV. The most opportune time to jump off a bandwagon is just before the next person jumping on tips it over. If the accelerating movement toward value-based payment (VBP) models in healthcare could be metaphorically thought of as a bandwagon, then its passenger weight increased dramatically this week with two major announcements.
The most opportune time to jump off a bandwagon is just before the next person jumping on tips it over. If the accelerating movement toward value-based payment (VBP) models in healthcare could be metaphorically thought of as a bandwagon, then its passenger weight increased dramatically this week with two major announcements. Je Suis Charlie? That all depends. Am I Charlie, a faceless Parisian joining with thousands of others along the Avenue des Champs-Élysées in candlelit vigil mourning a national tragedy? Or am I Charlie, a major newspaper like the New York Times having to carefully weigh my support of free speech – however rancor and callous that may be – against my potential complicity in unwittingly embracing and spurring additional tragedy? Either way, it’s no fun being Charlie.
Je Suis Charlie? That all depends. Am I Charlie, a faceless Parisian joining with thousands of others along the Avenue des Champs-Élysées in candlelit vigil mourning a national tragedy? Or am I Charlie, a major newspaper like the New York Times having to carefully weigh my support of free speech – however rancor and callous that may be – against my potential complicity in unwittingly embracing and spurring additional tragedy? Either way, it’s no fun being Charlie.

The core challenge is in the one size fits all model of healthcare that currently exists. The system as a…
Reblogged this on rennydiokno.com.
I think you're absolutely right, Scot. We've passed the point of no return on Federal dysfunction.
It sounds like violence can change one's mind about what is right and what is wrong. I always thought that…
The important issue is not the comment that Gruber made rather the fact that he and the administration intended to…